The planning of complex neurosurgery has taken a qualitative leap with the arrival of 3D-printed brain models. These physical replicas, created from the patient's medical images, offer surgeons an unprecedented preoperative planning tool. Before entering the operating room, they can visualize, manipulate, and practice the procedure on an exact and tangible copy of the patient's unique anatomy, which translates into greater safety and better clinical outcomes.
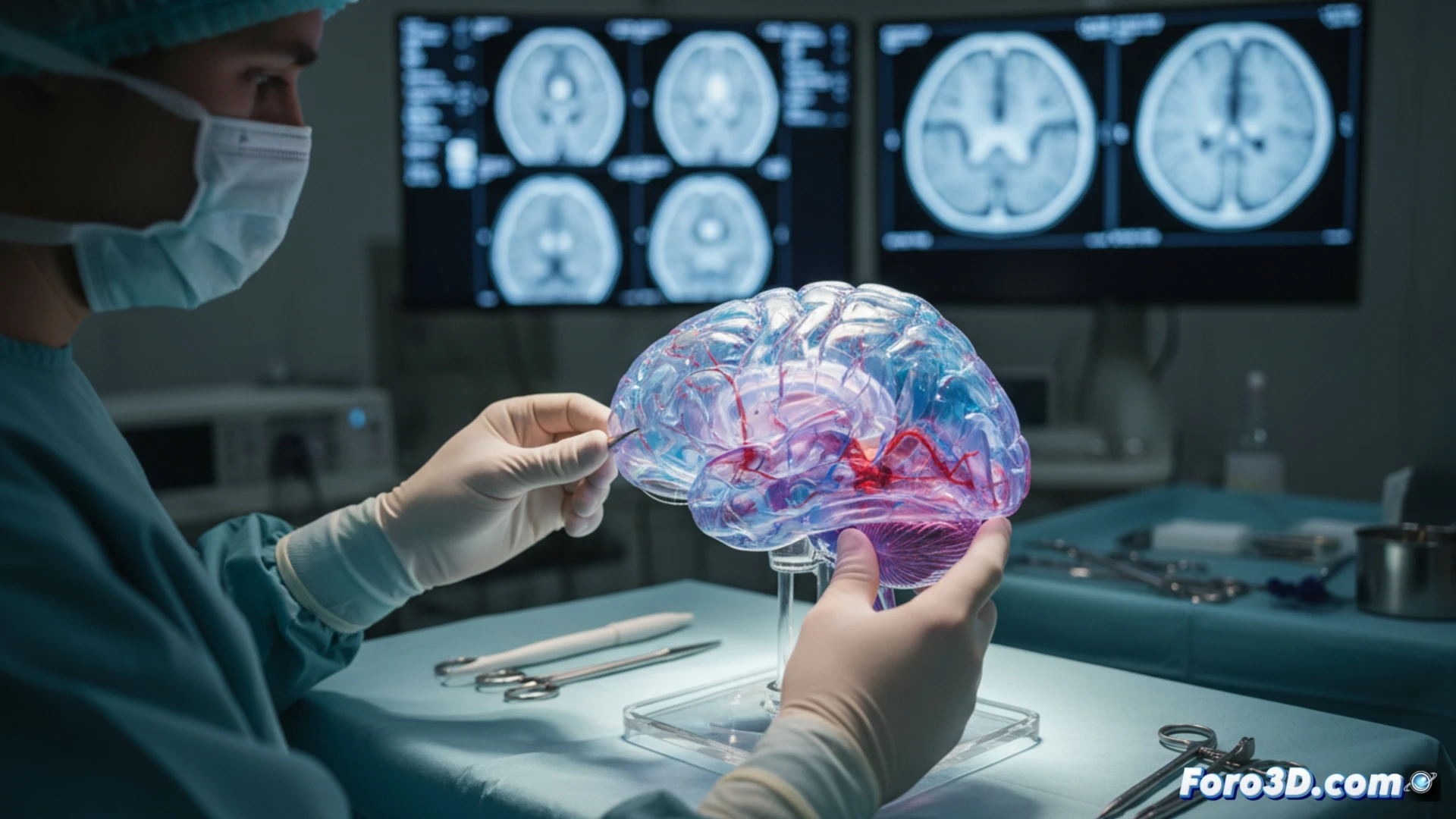
From scanner to operating room: the 3D biomedicine workflow 🧠
The process begins with the patient's MRI or CT scan data. These DICOM files are processed with specialized software to segment and isolate the brain structures of interest, converting them into a 3D digital model ready for printing. The choice of material, from rigid to flexible resins, depends on the need to simulate different tissues. This physical model not only allows planning the approach and rehearsing the surgery, reducing intraoperative time and risks, but also serves as an exceptional tool for explaining the procedure to the patient and their family.
Beyond innovation: tangible impact on clinical practice ⚕️
The adoption of this technology, exemplified in projects from institutions like the Bauhaus University of Weimar, marks its transition from prototype to operational tool. Its true value lies in integrating digital innovation with the most traditional surgical principle: know the terrain before acting. By offering anatomical precision and the possibility of rehearsal, these models are redefining standards of safety and efficacy in the operating room, paving the way for truly personalized and predictive neurosurgery.
How are 3D-printed brain models transforming preoperative planning and patient communication in highly complex neurosurgeries?
(P.S.: and if the printed organ doesn't beat, you can always add a little motor... just kidding!)